This page is a work in progress. It is clear DEE-SWAS information that stays true to research, but is easier and quicker for everyday people like myself to read, understand and explain. I also want to find a way for people to translate accurately into other languages. If you have ideas to improve this page or make DEE-SWAS clear, email melanie@voicesofdeeswas.org
The rare epilepsy that rewires a child’s brain during sleep
-
Why are there so many names?
You might feel confused about why there are so many names for this.
When my child was first diagnosed, we were told it was CSWS or ESES.
A year or two later, when I read more, I started seeing DEE-SWAS.
Now I understand that my child has EE-SWAS.
In online groups, people use different names. This can depend on what their doctor says, or when their child was diagnosed.
All of these names describe very similar conditions.
So what’s going on?
Over time, doctors have named different parts of the same thing:
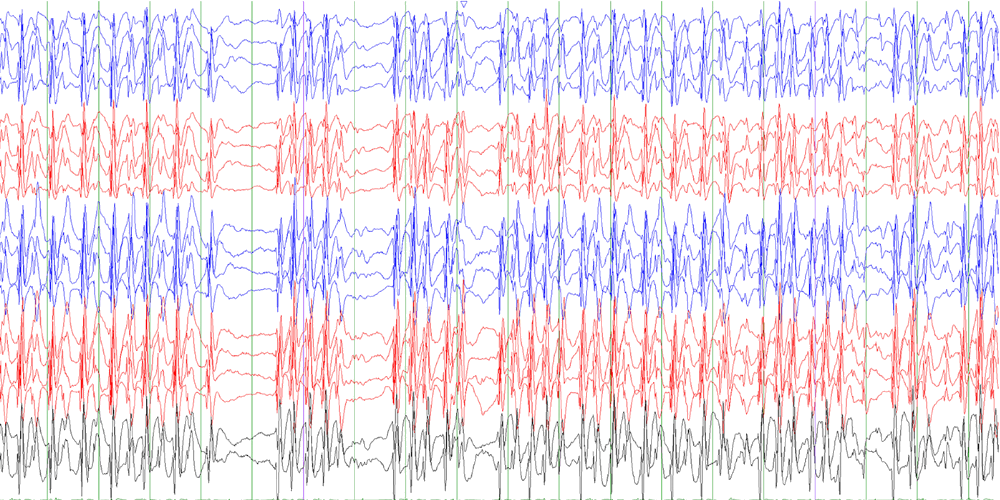
ESES / CSWS describe the brain waves seen on an EEG in sleep
Landau-Kleffner syndrome is a type that mostly affects speech
Newer names like DEE-SWAS show this is not just epilepsy - it also affects how our children learn, grow and change over time.
Why hasn’t this been made simpler for us?
Doctors working in this field trained at different times when different names were used - they’ve held on to the name they were taught
As a result, studies they do also use different terms
Some doctors prefer more specific labels. e.g. A doctor might use Landau–Kleffner syndrome if speech is the main issue.
How it affects patients and families
This can make it hard families to find clear health information, feel confident the information we find relates to our child’s diagnosis, and make sense of what it means for their day-to-day life.
It can also make it harder to explain to the important people in your child’s life.For example, your child might be diagnosed with CSWS, but the most helpful online health information to share with their teacher is written under DEE-SWAS.
Educators are busy and the simpler we can make it to support our child, the more confident we feel that our child can get the support they need at school.
-
1920s to 1930s
Brain waves are discoveredEarly EEG research made it possible to recognise this condition.
1924 – the first human EEG was recorded
Hans Berger (1873–1941) and The Discovery of Clinical Electroencephalography1935 – this is when the spike–wave activity in epilepsy (including DEE-SWAS) was first described.
A brief history on the oscillating roles of thalamus and cortex in absence seizures
1970s
Sleep shown to be importantThis is when doctors discovered that unusual brain activity during sleep can cause learning, communication and behaviour changes.
1971 – Doctors described ESES in children who had lost skills
Subclinical "Electrical Status Epilepticus" Induced by Sleep in Children
1970s to 2000s
A condition is recognisedDoctors begin to name this as a syndrome linked to:
abnormal brain activity in sleep
loss or slowing of skills
changes in behaviour
ESES and CSWS become the names used. The focus goes from seizures alone to how a child is learning and developing. No clear cause recognised.
Subclinical "Electrical Status Epilepticus" Induced by Sleep in Children2000s to 2010s
A spectrum is recognisedDoctors see CSWS/ESES is not one condition, but a range, with different ways it shows up and how the child changes over time.
This includes overlap with:
Landau–Kleffner syndrome (LKS)
focal epilepsies with sleep activation
Guidelines for EEG in encephalopathy related to ESES/CSWS in children
2013
First gene link foundIn 2013, a gene called GRIN2A was discovered to be a cause in some children with conditions like CSWS and Landau–Kleffner syndrome. This was one of the first clear genetic links.
GRIN2A mutations cause epilepsy-aphasia spectrum disorders
Question: when were other causes identified - perinatal stroke, cortical malformation, other brain injuries, immune system
2010s to present
New namesEarlier names like ESES and CSWS were about what the EEG pattern looked like.
But they didn’t always match the impact in children.Newer terms focus on how the child is learning and developing in their day-to-day life.
Common names today:EE-SWAS - used when a child develops typically at first, then loses or slows skills
DEE-SWAS - used when there are already differences in a child’s development, and epilepsy adds further impact.
Proposed classification: Syndromes in Children
2020s
Brain networks and connectionsThe focus is now moving beyond seizures and EEG patterns.
Newer research suggests DEE-SWAS is not just about abnormal activity in one part of the brain. Changes in how brain networks develop and work together over time may help explain changes in learning and development.
Developmental and epileptic encephalopathy with spike–wave activation in sleep: From the ‘functional ablation’ model to a neurodevelopmental network perspective -
What the research says
A recent paper, Rebuilding the Tower of Babel: The Current Landscape and Emerging Opportunities in DEE-SWAS, shows that:
There is still no global agreement on how to diagnose DEE-SWAS.
The main marker used is the spike-wave index (SWI), measured on an EEG. But experts do not agree on how to use it.
There is no consistent cut-off for how much of sleep must be affected. There is also no clear evidence that one number is correct.
“The historical 85% cutoff has been predominant, but proposed guidelines in 2009 offered a lower cutoff of ≥50% in NREM sleep. Some groups utilize a 25% cutoff.”
There is also no standard way to calculate SWI. Different clinicians use different methods, which can give different results.
There is no clear agreement on what SWI actually means in real life, or how well it reflects what is happening to the child.
Tower of Babel idea
The title of the paper uses the story of the Tower of Babel.
In the story:
People are trying to build something together
But they suddenly speak different languages
They can no longer understand each other
The project breaks down into confusion.
In this paper, Tower of Babel means:
People are using different terms, definitions and methods, so they cannot clearly communicate or move forward.
Why this matters for families
The lack of agreement about SWI (for example 85%, 50% or 25%) can affect whether a child:
is diagnosed
receives treatment
is monitored closely
is seen as having a serious condition.
As one paper states:
“Due to the lack of an established electroclinical phenotype, there has been no standardization of therapy.”
The same child could be diagnosed in one clinic, and not in another, based only on how SWI is measured or interpreted.
A child may be diagnosed with DEE-SWAS when their SWI is above a certain level. But if it drops below that level, they may no longer be considered to have it.
This can happen even if:
thinking and learning are still affected
cognitive difficulties continue
behaviour and emotional regulation are still impacted
Questions this raises
How much do these cut-offs reflect a child’s needs - and how much do they reflect what each health system can support?
What happens to children who fall just below a cut-off, but are still struggling?
What families experience
Families may face:
different answers from different clinicians, with no clear way to resolve them
long delays before changes are recognised or acted on
ongoing learning and behavioural difficulties without a clear diagnosis
access to care and support that depends on cut-offs, not need.
Parents and carers often have to advocate again and again just to have concerns taken seriously.
This comes with a real cost in time, energy and emotional load.
Access also depends on where you live
Where a child lives can affect the care they receive.
A child may be seen by:
a neurologist with deep experience in developmental and epileptic encephalopathies
or a clinician who has rarely if ever seen DEE-SWAS.
The bottom line
The paper makes this clear:
We still don’t have a shared and reliable way to define, measure and diagnose DEE-SWAS.
Until there is global agreement on SWI:
diagnosis will continue to vary
decisions will differ between clinicians and services
Children may live with lifelong effects from decisions made - or not made - at critical times.
Families will continue to carry deep uncertainty that affects their child’s care, future planning and daily life.
-
Developmental and Epileptic Encephalopathy with Spike–Wave Activation in Sleep (DEE-SWAS) is an umbrella term for a rare type of childhood epilepsy, with varying presentations, causes and outcomes.
It affects around 1 in 200 children with epilepsy.
It usually starts between ages 2 and 12, most often around 4 to 5 years old.
Children can lose previously learned skills, or their development may slow or stop, meaning they are not gaining new skills as expected.
This is linked to unusual brain activity during sleep.
More information
If you’re looking for more detailed medical information about DEE-SWAS, these pages may help.They can be technical, but they provide more in-depth explanations of diagnosis, EEG patterns and treatment.
-
The less the environment around a child can adapt to their changing needs, the harder life becomes.
Impact on learning, connection and participationCommon challenges families talk about include:
Cognitive
Regression in thinking, problem-solving and memory
Difficulty learning and retaining new information
Impaired attention span and focus
Poor planning and decision making (executive function)
Slowed processing speed.
Language and Communication
Delayed or halted speech
Loss of previously acquired words or sentences
Difficulty understanding spoken language (receptive language)
Difficulty expressing thoughts verbally (expressive language)
Limited vocabulary
Trouble with articulation and clarity of speech
Social communication challenges (e.g conversations, social cues)
Emotional wellbeing
Hyperactivity or impulsiveness
Mood swings, anxiety, depression
Difficulty in emotional regulation (e.g., sudden outbursts)
Social withdrawal and lack of interest in social interactions
Aggression or irritability
Repetitive behaviours or routines
Difficulty adapting to routine changes
Reduced ability to express emotions.
Movement and coordination
Coordination and balance difficulties
Delay or loss of gross motor skills (e.g., walking, running, jumping)
Fine motor difficulties (e.g., writing, buttoning clothes)
Tremors or abnormal movements
Muscle weakness or stiffness (hypertonia)
Ataxia (uncoordinated movements)
Gait abnormalities (e.g., walking difficulties, unsteady walking).
Seizures
Subclinical seizures in sleep, especially in slow wave (deep) sleep (spike-and-wave activity)
Subclinical seizure activity in the waking hours
Occasional or frequent clinical seizures, including visible (e.g., tonic-clonic, absence) both day and night
Toileting and continence difficulties
Bedwetting
Accidents in the day.
Sensory and Perception
Sensory processing(hypersensitivity or hyposensitivity)
Sensory overload or under-reactivity (e.g., to sound, light, touch)
Difficulty with spatial awareness and body positioning
Impaired vision or hearing processing (e.g., trouble interpreting visual or auditory stimuli).
Social and Interactive
Difficulty forming and maintaining friendships
Struggles with peer relationships and social integration
Lack of interest in group activities
Trouble understanding or responding to social cues (e.g., tone of voice, facial expressions)
Isolation or avoidance of social situations
Reduced ability to engage in age-appropriate play or interactions
Sleep
Sleep disturbances (e.g., trouble falling asleep, frequent waking)
Irregular sleep habits (e.g., staying up late or waking up too early)
Sleep apnoea or irregular breathing patterns during sleep
Restlessness or hyperactivity at night
Poor sleep quality despite adequate hours of sleep.
Co-existing conditions
Intellectual disability (ranging from mild to severe)
Autism spectrum disorder (ASD)
Attention deficit hyperactivity disorder (ADHD)
Cerebral palsy
Speech and language disorders
Sensory processing disorders
Sleep disorders (e.g., night terrors, insomnia).
-
To come
-
Making sense of it
(for yourself and others)

-
The brain of a DEE-SWAS child is a library without a librarian.
Picture the brain as a library – a place where books (representing thoughts, memories, and knowledge) are carefully stored and organised. Normally, each night, as we sleep, the brain works like a diligent librarian – sorting, storing, and making sure everything is in its right place.
But in the case of Developmental andEpileptic Encephalopathy with Spike-Wave Activation in Sleep (DEE-SWAS), the process goes awry. Imagine the librarian doesn't turn up for work. Without their organisation, the books get left scattered all over the place. In the brain, this translates to the spike-wave discharges disrupting sleep, preventing the brain from properly organising and consolidating memories and learned information.
The result? Just like a library with books in chaos, the brain’s ability to store, retrieve, and build on knowledge is compromised. This leads to cognitive and developmental challenges, affecting learning, memory and overall brain function.
In short, DEE-SWAS is like a library without a librarian during crucial sleep periods – the brain simply can’t get its act together, and the outcome is a disorganised, inefficient cognitive system.
This concept is something that stuck with me that a parent in an online support group shared. If you read this, and that person is you, please let me know so I can credit you for the idea. -
It can feel like a child is carefully knitting something during the day in their mind. Stitch by stitch, they are building skills, memories and understanding.
But overnight, something begins to pull at the yarn… quietly undoing what was learned that day.
Some nights only a few stitches loosen. Other nights, whole sections of hard work are undone.By morning, the knitting is no longer what it was when last left. Parts may need to be repaired, or may be gone altogether.
Each child’s knitting pattern is different, and what unravels, and how much, is not the same for everyone.
This concept is something that stuck with me that a parent in an online support group shared. If you read this, and that person is you, please let me know so I can credit you for the idea. -
Imagine trying to sleep while someone repeatedly flicks the lights on and off in your room. Just as you drift off, the light snaps on again. Then off. Then on.
This continues for hours.
By morning, you haven’t truly rested. You might feel irritable, confused, slow to respond, or unable to think clearly.
Now imagine this happening night after night, for months or years.
This is one way to understand what disrupted sleep in DEE-SWAS can feel like for a child.
This concept is something that stuck with me that a parent in an online support group shared. If you read this, and that person is you, please let me know so I can credit you for the idea.